This is an account of things during my recent surgery. NOTICE: Although most of this will not contain anything horrible, there might be a few photos that would be bothersome to those who are bothered by such things.
On 27 November, I ate some late breakfast and settled in to watch football. But by about 2pm, I was having intense pain in my left shoulder, seemingly above the collarbone. Actually, I'd been having similar pains for several years, typically after eating. Such pain is symptomatic of acid reflux disease, but it also a symptom of some myocardial infarctions (MIs) - heart attacks. This time, no antacids were effective and the pain, stronger than ever before, continued without letup. Vickie was concerned because the pain was so persistent and intense, fearing it might indeed be an MI. Finally, I relented in my resistance to seeking medical aid and so, after one false start, we were on our way to the Emergency Department (ED) at Norman Regional Hospital. Thus, began my first experience with major surgery. This is a relatively brief story of my stay in the hospital and all the experiences springing from it.
Although this was (and continues to be) an experience I would rather not have had, like much of life, it also produced some positive moments, and I want to share those as well. Spending nearly two weeks in the hospital (I was finally discharged on the evening of 08 December) gives one a great deal of time alone to ponder things and I feel obligated to share at least some of those ponderings.
So, anyway, there we were in the ED, with me vomiting, uncertain about what was the cause of my pain and discomfort. Clearly a series of tests was called for, which began in the ED with an electrocardiagram (EKG). The early indications were negative regarding an MI, which was encouraging, but that left open the question of what was going on. So, I was admitted to the hospital, in room 2067 of 2 West (the so-called "telemetry" wing, which maintains continuous electronic but wireless monitoring of heart and respiration). On the next day (Sunday), I had a CT scan and ultrasound imaging that resulted in a definitive diagnosis. I had a hiatal hernia - in this case, a relatively rare example called paraesophageal hernia, in which a substantial part of my stomach had moved into the thoracic cavity. There was concern about loss of blood flow to the stomach, suggesting a sense of urgency to the now-inevitable surgery, because if there was a loss of blood flow, and it persisted, I would lose some or all of the stomach! Note that hiatal hernia is also closely associated with acid reflux. At any rate, it was decided to delay the surgery to the next day, and I was finally put on IV fluids late on Saturday to try to re-hydrate me before the operation. Dr. Tom Connally was my surgeon of choice, which turned out to be an excellent one. My regular physician, Dr. Hal Belknap (also my good friend) was also involved, naturally.
Monday morning (29 November) it was off to my great adventure - I talked briefly with Dr. Connally in the holding room before being wheeled into the operation. The next thing I remembered is waking up in my hospital room! I was as if no time had passed between talking with Dr. Connally and waking up in my room - apparently, the anesthetic can cause some retrospective amnesia. I have no memory of actually going into surgery room at all. Very strange, but not entirely bad, either.
The operation apparently went well enough, and took about 2 1/2 hours. I was in only a little pain and apart from being woozy, things seemed o.k. The surgery apparently involved some need to push forcefully on my ribs to make room for things to happen and I had some bruising from that treatment. The incision ran from the xyphoid process (just below the sternum) to just above my navel, and a gastric tube was left inside, protruding from my side. It's still there as I write this. The tube was not for drainage, although it served that purpose for a few days post-op, but to anchor my stomach into the lower abdominal cavity - to keep if from migrating back up from whence it had just come. This tube is to stay in for several weeks but will eventually come out. It was capped off and I could begin to actually eat and digest solid food by Thursday, post-op.
On the Tuesday following surgery, I was taken away for an echocardiagram - basically an infrasound examination of the heart. This had been ordered on Saturday, but was not actually done until after the hernia surgery. This seemed rather unnecessary, but it did give final confirmation that there had been no MI, so I suppose it wasn't without value, although it certainly had its price in $$ (like everything associated with this episode!). By Tuesday, it was also apparent that I was coughing up blood, and it was confirmed after an X-ray that I had caught pneumonia as a complication from the surgery. This rather serious issue forced me to say in the hospital for an extra week, and massive IV doses of antibiotics began that continued right up to my discharge. For the first few days, nothing seemed to be happening, but gradually the pneumonia began to decline and by the weekend, I was ready to go home. Dr. Camp (a respiratory specialist called in because of the pneumonia) said I needed to stay the full week course of the antibiotic that could not be taken orally. Hence, my stay was longer than I hoped for, but eventually my incarceration ended and I was able to return home, where my recovery continues.
29 Dec update: In response to several questions, I asked Dr. Connally about the "cause" of my condition. He believes it largely to be a congenital problem and says that it's unlikely there is anything I could have done to mitigate the eventual need for the surgery. Apparently, I was predisposed to this and once it began, it was only going to get worse - which seems quite consistent with my experience. Even coming in earlier would not have changed anything about the eventual need for surgical intervention of just the sort that was done. I'm simply glad it happened when it did, and not on some trip of mine (I had just returned from a week in Beijing the week before I went to the hospital!). The gastric tube is now out and the hole in my stomach is apparently healing rapidly, as predicted. I have several more follow-up appointments in the next few weeks.
04 Apr update. The healing continues. I'm now in the process of paying off all the remaining bills, of which there have been many. I have a stack of paperwork, of course. It seems that my health insurance has taken a major hit from all this. With the exception of the deductible part of the bills, for the most part my co-payments have been numerous but relatively small. The total costs of this process have been staggering. I'll resist the temptation for a rant about the cost of medical care - that would be pointless. I've had enough follow-up tests and procedures done (including a colonoscopy!) to add significantly to my bills, most of which have been paid by the insurance, thank goodness. Basically, I seem to be O.K... and things are functioning more or less normally.
Since my wonderful wife Vickie is a Registered Nurse, I have known more than most people about the realities in any hospital. Like any large organization, they have both fabulous dedicated employees, and uncaring incompetent employees, as well as everything in between - this came as no surprise to me, therefore. At the outset, I want to say that the vast majority of the employees are wonderful and I received excellent care, overall. But I also observed firsthand some of the reasons why hospitals are not necessarily ideal places for rest and recovery.
I had a private room, which was a great luxury, but I never could get very comfortable on the bed. The room's door needed to be firmly closed or it wouldn't stay closed. Most of the people coming and going, of which there were hordes at times, could hardly ever get the door properly shut, which would then swing to mostly wide open. The hall outside my room was noisy for a considerable period every day, and it seemed remarkable to me how thoughtless some people could be with loud talking in the halls, even during the wee hours of the morning. My sleep schedule was hopelessly disrupted, and remains so as I write this.
At night, when things quiet down (more or less), the relative calm can be broken by "code blue" calls on the intercom - someone is either in cardiac or respiratory arrest and this is a call for immediate aid that goes out to everyone within reasonable distance of the code. Running feet down the hall usually follow such a call. It's a reminder that death stalks the halls of any hospital. Although such events would make me grateful that I was as well off as I was, they also include a reminder of what could be. All it takes is a stray germ somewhere and a fatal case of pneumonia could ensue. Since I had pneumonia, that was a particularly troubling thought. Hospitals are dangerous places, no doubt. Staying there alone at night was often a time to reflect on death - for me anyway.
I don't believe I have any morbid fear or fascination with death. Over the years, it becomes apparent to anyone who lives to my age that people die, and that one day your own turn will come. Far from invoking fear, such thoughts usually make me realize how fortunate I've been, in so many ways. This time, I had pneumonia, however, and I was aware that death could indeed be on my doorstep. I could imagine how it would happen and what effects it might have. Suddenly, some of the things that had been going on in my life seemed much less important than they had been. I'm not going to dwell on these personal issues here, but I think I finally was reconciled to some things from my past that had been troubling to me. I resolved to put them away when I got out of the hospital, and I am in the process of doing so. It actually is a relief and it makes me sad to think how much of my life was wasted being upset about these past events.
Like any other human endeavor, it became clear to me that hospitals struggle with getting information to the people who need it. Like my delayed echocardiagram, I found that orders and information about diagnosis from the doctors were often slow to get to the nurses and to the various departments of the hospital. It seems to me that with the widespread use of computers in hospitals nowadays, this should be less of a problem than ever, but during my stay, it seemed just the opposite was true. Since Vickie spend a good deal of time with me during most of stay, and she is currently working as a house supervisor, I think even she learned some new and sometimes disturbing things about information flow. Although information flow is a problem in most enterprises, a hospital deals with life and death issues every day - the importance of getting information to its intended locations in a timely way is thereby magnified. Far be it from me to tell folks in hospitals how to do their jobs, but I think I am entitled to offer this opinion based on the evidence I saw.
It was also interesting to see how much variation there is in doing IV "sticks" - either for laboratory blood work or for IV therapies. Being a professorial sort, I gave out "grades" to the folks doing this and they ranged from "A" to "F" When you get bloodwork done virtually every day for several days, your veins can end up pretty abused. I make no claim that I could do this at all, much less do it better than the folks who were on the job, but again - it's an observation that assumes some significance for extended hospital stays.
Hospitals are legendary for being lousy places to rest. For the most part, I concur with this assessment, but I have to temper that with the observation that my nurses did an excellent job of minimizing the times my rest had to be interrupted. For the most part, this aspect of my stay was perhaps slightly better than I expected. Of course, it still was difficult to rest.
Whatever my limited gripes might be, for the most part, I was given excellent care by the nurses and aides. It was nice to know their names, which were written on a whiteboard in my room at each shift change. Most of them were working very hard and yet never hesitated to respond to my requests with a smile. Thank you, one and all. The list of photos at the end is by no means exhaustive of those who contributed to my relative comfort during my stay.
I was shocked at the outpouring of get-well wishes and even outright gifts that people sent or brought,. It actually makes me somewhat embarrassed or even ashamed to realize that I may not always have responded in such a generous and thoughtful way to news about the misfortunes of my friends and family. Vickie did send out some emails to a few people right after I was admitted and it seemed like the whole thing sort of snowballed. I wound up with a window full of flowers, extra things to read, cards, phone calls, emails, and a substantial number of visits. What did I do to deserve such good friends and caring family members? I don't understand this, and I have to say I was overwhelmed. Several people apologized for not coming to visit, but they had various potentially infectious ailments that they were sparing me from - I appreciate the sentiment this implies, and also I really did not need any more complications! The nurses and aides were pretty impressed with all the stuff in my room and thought I must be someone important. Well, no person with such friends and family can ever be said to be poor or unfortunate. I'm proud to know such people and this experience has underscored the feelings I have had over recent years - I'm so blessed because of my friends and family. I don't think I took this completely for granted before, but my experience has magnified my sense of gratitude. I hope that whatever I've done actually merits such treatment, but I will work even harder to make sure that you all know how much I need and appreciate your support - and to give it back to others who may need it as much or more as I did during this brief crisis in my life.
First and foremost among this group was my wife, Vickie. I've known she's a great nurse for many years, based mostly on second-hand, and therefore more objective, testimony. Her lengthy stays in my room, including several overnighters, made the whole experience so much easier to bear and she seemed to know just what I needed even before I did. I've heard such things about her from people who have been her patients, but this time I got to see these things first hand. I don't believe I've ever done anything to deserve such a fantastic spouse, but I hope I'm smart enough to keep that in mind and do everything I can to keep her fooled. She sacrificed a lot to be with me for that time in the hospital, and it made a real difference in my stay. Clearly, the young nurses all looked up to her, as both a storehouse of practical nursing knowledge and as a role model and mentor. I've always been proud of her and what she does, and cannot begin to say how important she has been in all the good things I've been able to do. This stay underscored how much I need her and love her.
Thank you one and all for your thoughts and wishes on my behalf. It has made something that might seem to many as a physical ordeal turn into something wonderful. I hope none of you need such an experience to make you see how fortunate you are, but that's what has happened with this for me. You are all blessings in my life and I treasure my time with you, however poorly I may demonstrate it.
And thanks to the doctors, nurses, aides, and staff associated with Norman Regional Hospital, and especially the folks staffing 2 West. I will never want to spend more extended stays in any hospital, but I appreciate the efforts expended to make my stay as bearable as possible.
I feel great and the symptoms I'd been having for years are now just a bad memory. Followup tests have been positive, so I'm now more or less back 100%.
All of these were taken by Vickie. Click on the thumbnails below to see larger versions.
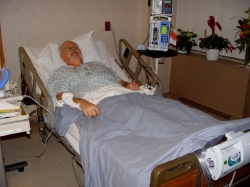
Me, in my normal position, with the IV pump at my left side
Me, with oxygen and IV tubes in
A window full of flowers and gifts!
Reading emails on my laptop
Dr. Belknap, doing his thing
Nurse Aaron, with his good sense of humor showing
Nurse Jamie
Aide Anita
Nurse Cindy
Dr. Connally, wearing his typical smile
Dr. Camp, at work. His treatment of my pneumonia was responsible for me staying an extra week, but it worked!
Aide Mumbali, grinning as usual
Clinical Nurse Specialist Kela
Nurse Kendra
Nurse Jennifer
The scar (and gastric tube)
Even my son sent flowers, from Baghdad! These were waiting for me at home - I have a great family!!.
And the scars, with the bandages removed - in early February. I hope Dr. Connally is proud of his work!! Sorry, but this is just necessary. The round scars at the top are the remains of very nasty blisters from the tape bandages. The main scar remains prominent as of 04 April, but the blister scars have pretty much disappeared and the gastric tube hole to the stomach scar is getting smaller and less prominent than shown here.